Biocompatible Materials: The New Standard in Orthodontic Appliances
As orthodontic appliances spend weeks or months in the oral environment, the biocompatibility of materials is more important than ever. New materials are raising the bar for safety and performance.
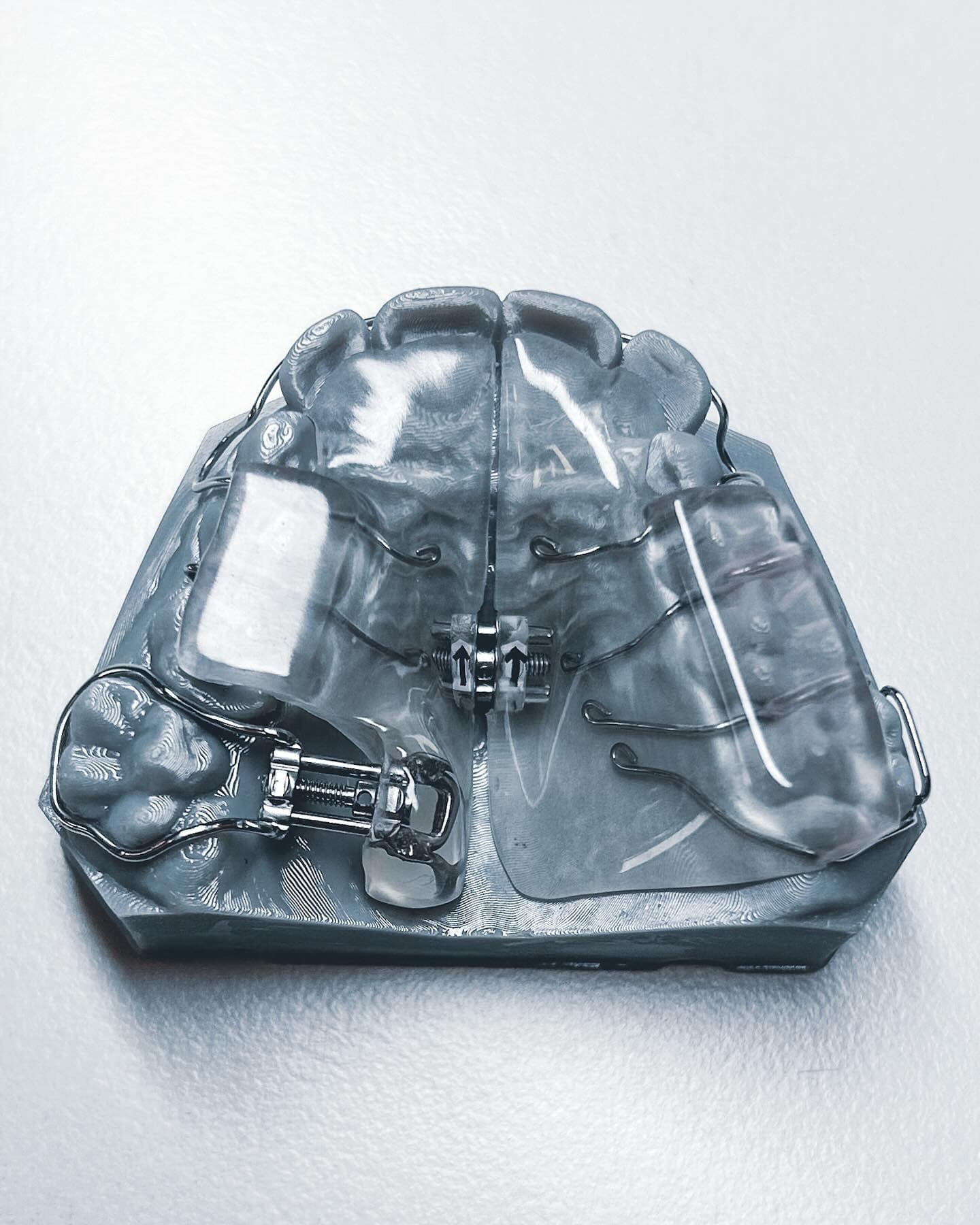
Why Materials Matter More Than Ever
Orthodontic appliances are medical devices that spend extended periods in direct contact with oral tissues. Aligners are worn 20+ hours daily for months. Retainers may be used for years. Splints are worn nightly for extended periods. The materials these appliances are made from must meet rigorous standards for safety, durability, and clinical performance.
As the orthodontic industry shifts toward digital manufacturing — particularly 3D printing — the range of available materials is expanding rapidly. This expansion brings both opportunity and responsibility: more options for performance optimization, but also a greater need to verify that every material meets the biocompatibility standards patients deserve.
What "Biocompatible" Actually Means
Biocompatibility isn't a single property — it's a comprehensive assessment of how a material interacts with living tissue. For orthodontic materials, this typically includes testing for:
- Cytotoxicity — Does the material harm cells on contact?
- Sensitization — Does it trigger allergic reactions?
- Irritation — Does it cause inflammatory responses in oral tissues?
- Systemic toxicity — Are there harmful effects if trace amounts are absorbed?
- Genotoxicity — Does the material interact with DNA in ways that could cause mutations?
These assessments follow international standards, primarily ISO 10993 (Biological evaluation of medical devices), which provides a framework for testing that's recognized globally.
For a material to be used in orthodontic appliances, it should meet these standards and carry the appropriate regulatory classifications — typically Class I or Class IIa medical device material designations in the EU (under MDR) and FDA clearance in the United States.
The Material Landscape in 2026
Thermoplastics for Thermoforming
Traditional aligner and retainer materials are thermoplastic sheets — PETG, polycarbonate, polypropylene, and multi-layer composites. The latest generation includes:
- Zendura FLX — A multi-layer material that delivers sustained gentle forces with improved comfort
- Essix ACE — A copolyester known for clarity and durability
- Duran+ — Enhanced PETG with improved crack resistance
These materials are well-established and have extensive clinical track records. They're BPA-free, phthalate-free, and meet applicable biocompatibility standards.
3D Printable Resins
The rapid growth of direct-print orthodontics has driven demand for printable resins that match the safety profile of traditional materials:
- Graphy tera harz TC-85 — A photopolymer resin designed specifically for direct-print aligners. ISO 10993 certified, Class IIa medical device material.
- KeySplint Soft — A flexible resin for printed splints and guards
- Dental LT Clear — Formlabs' long-term biocompatible resin for splints and retainers
Printable resins undergo the same biocompatibility testing as traditional materials but face additional scrutiny because photopolymers require complete curing to ensure no residual monomers remain in the finished product.
Metals and Alloys
For fixed appliances, wires, and metal frameworks, the standard materials include:
- Medical-grade stainless steel — The workhorse for brackets, bands, and wires
- Nickel-titanium (NiTi) — Superelastic wires with shape memory properties
- Cobalt-chromium — Used for specialized frameworks and components
- Titanium — Biocompatible option for patients with nickel sensitivity
The Lab's Role in Material Safety
Orthodontic laboratories play a critical role in material safety — not just in selecting certified materials, but in processing them correctly. For 3D printed appliances, proper post-processing is essential:
- Complete washing to remove uncured resin
- Full UV curing to ensure complete polymerization
- Appropriate sterilization before delivery
At NordicDens, every material we use carries appropriate certifications and documentation. Our post-processing protocols are designed to ensure that finished appliances meet the biocompatibility standards specified by the material manufacturers. We maintain material traceability records so that every appliance can be linked to its source material batch.
What Clinics Should Look For
When evaluating materials — whether directly or through their lab partner — clinics should consider:
- Certification documentation — Can the lab provide ISO 10993 test reports and regulatory clearances for the materials they use?
- Post-processing protocols — Does the lab follow validated washing and curing protocols for 3D printed appliances?
- Material traceability — Can the lab trace each appliance back to its material batch?
- BPA and monomer residual testing — For printed resins, has residual monomer content been tested and documented?
NordicDens Material Standards
We take material selection and processing seriously. Every material in our production workflow is:
- Sourced from established manufacturers with documented regulatory compliance
- Tested according to applicable ISO standards
- Processed according to manufacturer-validated protocols
- Traceable from raw material to finished appliance
As new materials enter the market, we evaluate them against the same rigorous criteria before incorporating them into our production capabilities. Innovation is important, but not at the expense of patient safety.
NordicDens is a modern orthodontic laboratory in Tallinn, Estonia, serving clinics across the Nordics and Europe with precision appliances and digital workflows.
Latest from the Blog

Technical Guide to Orthodontic 3D Printing Resins
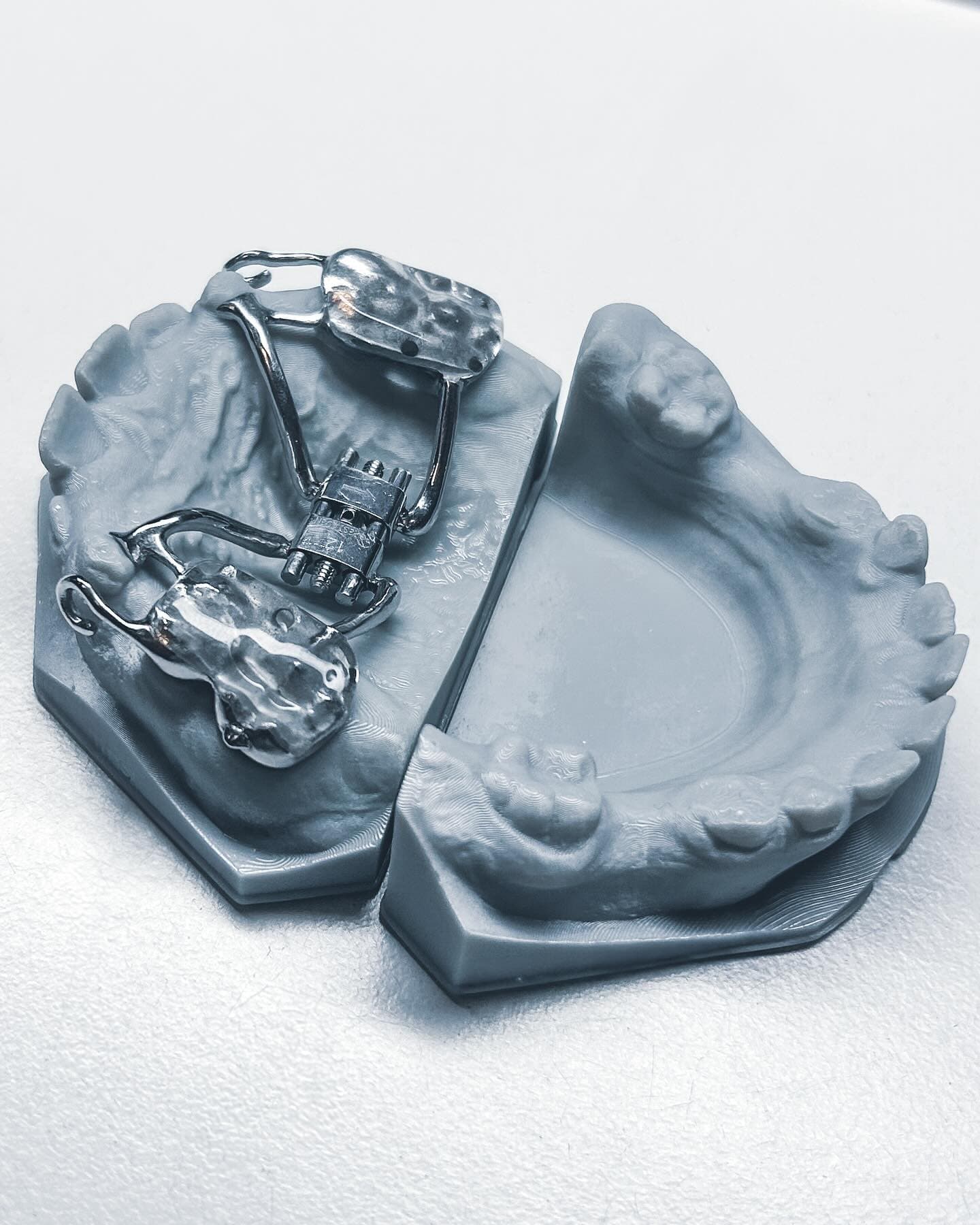
The 3D Printing Revolution in Orthodontics: What Every Clinic Should Know
From thermoforming bases to direct-print appliances, 3D printing has become the backbone of modern orthodontic lab production. Here's what clinics should understand about this shift.
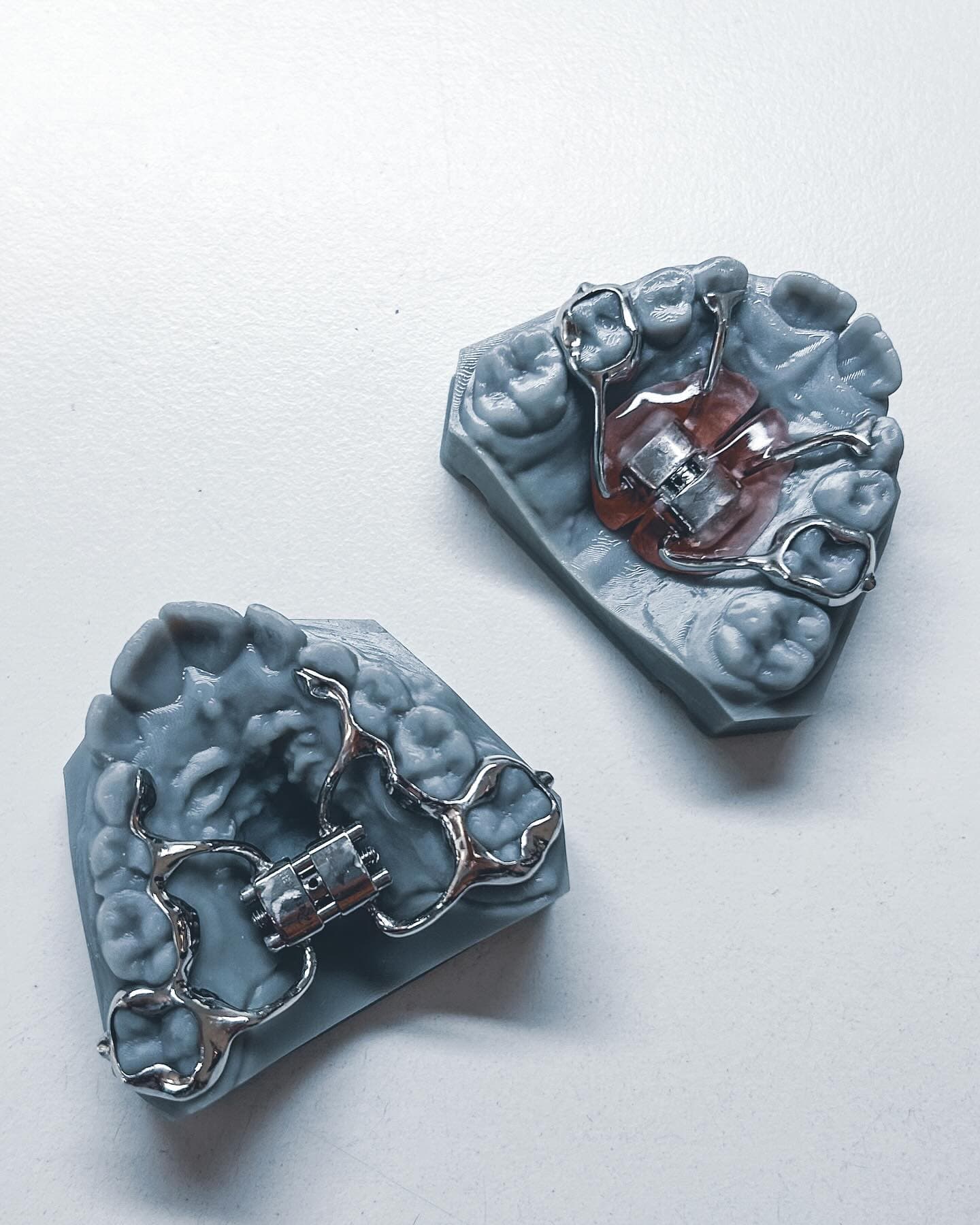
Digital Workflow: From Intraoral Scan to Final Appliance
The fully digital workflow has redefined how orthodontic labs and clinics collaborate. From the moment a scan is submitted to the final appliance delivery, every step benefits from digital precision.