The 40% Thickness Gap: How Thermoforming Impacts Aligner Performance

Thermoforming significantly reduces the nominal thickness of orthodontic materials, often resulting in a final appliance that is 15% to 40% thinner than the original plastic sheet. This thinning is rarely uniform, creating localized variations in stiffness that directly influence force delivery, tracking, and clinical predictability. As a clinician, you rely on the biomechanical properties of a material to move teeth, yet the 0.75 mm or 1.0 mm sheet you select is not the geometry the patient ultimately wears. Understanding the technical impact of the thermoforming process is essential for troubleshooting cases where the fit feels accurate but the tooth movement fails to materialize.
The Geometry of Thinning: Nominal vs. Effective Thickness
When a thermoplastic sheet is heated and drawn over a dental model, it undergoes substantial stretching. Research utilizing micro-CT and nano-CT imaging confirms that a sheet’s nominal thickness does not remain uniform after forming. The material must travel further to cover certain anatomical landmarks, leading to an inconsistent distribution across the arch.
Studies consistently show that thermoformed samples are notably thinner at the anterior teeth and gingival centers compared to posterior teeth and occlusal surfaces. This occurs because the material stretches most over the tallest or most prominent parts of the arch. For a detailed look at how these materials have evolved to handle these manufacturing stresses, you can explore the evolution of clear aligners and their transition into mainstream orthodontics.
Positive Pressure vs. Negative Vacuum
The specific method of thermoforming – whether using positive air pressure or negative vacuum pressure – radically alters the material’s final behavior.
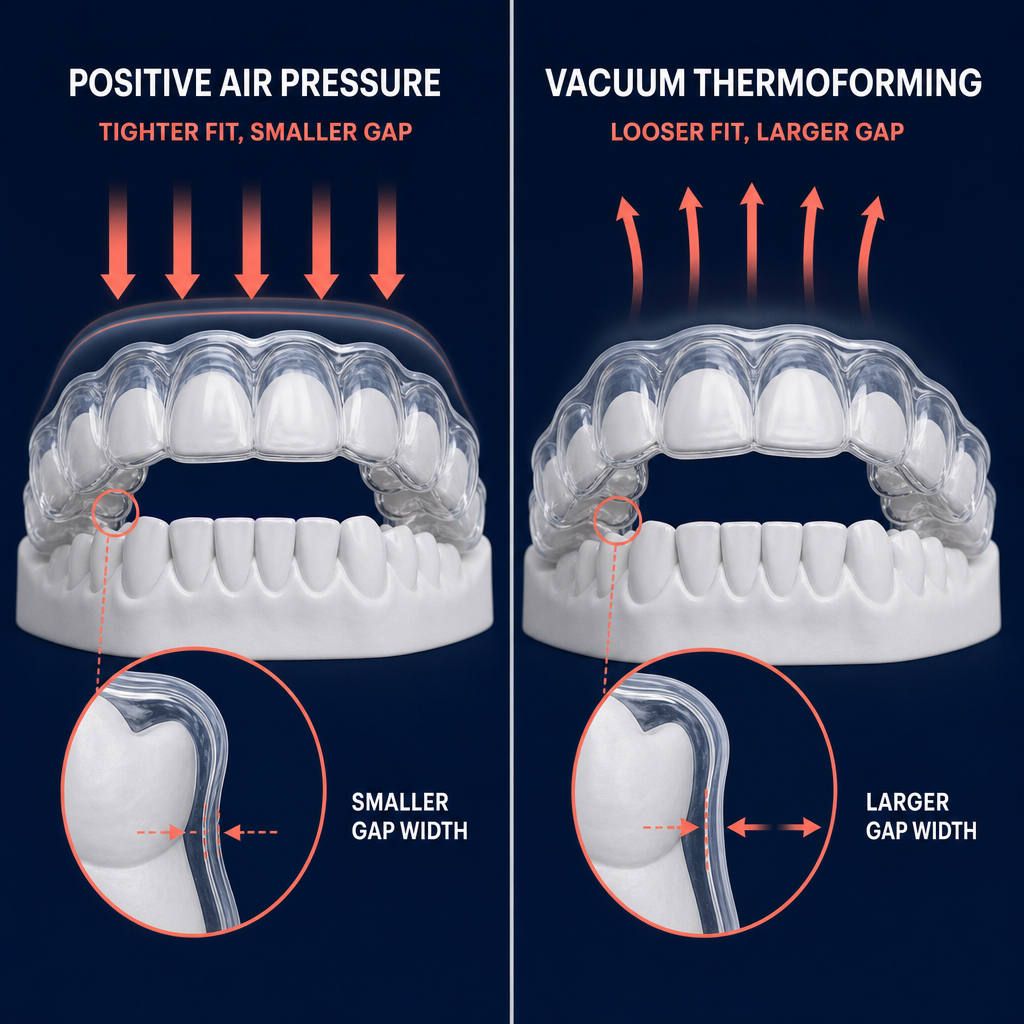
- Positive Air Pressure: This method generally produces higher force delivery and better adaptation to the model. By pushing the material onto the model with compressed air, the gap width between the tooth and the appliance is minimized.
- Vacuum (Negative) Pressure: This often results in slightly larger gap widths and less precise adaptation, particularly in deep interproximal spaces or complex undercuts.
The choice of machine and material also affects final translucency and thickness distribution. Some PET-G and multi-layer materials respond differently to heat, and choosing the right combination is a critical step in the digital workflow from scan to appliance to ensure predictable clinical outcomes.
Clinical Consequences of Thickness Loss
The thinning of the material is not just a technical curiosity; it has three primary clinical consequences that impact your daily practice.
Force Delivery Degradation
The force delivered by an aligner is proportional to the cube of its thickness. Consequently, a 20% reduction in thickness can lead to a nearly 50% reduction in the stiffness of the appliance. This explains why certain movements, such as root torque or bodily movement, may stall if the material thins too much in critical areas.
Fit and Gap Width
The gap width – the space between the internal surface of the aligner and the tooth – is influenced by how well the material recovers after being stretched. If a material thins excessively, it may lose the structural integrity required to grip the attachments or the clinical crown, leading to poor tracking and patient discomfort.
Material Fatigue
Thermoforming alters the physical and mechanical properties of the polymer worldwide. The heating cycle can induce internal stresses, making the material more susceptible to intraoral wear and chemical degradation over the typical wear cycle. This degradation can lead to loss of retention before the patient is ready to switch to the next tray.
Addressing the Variability of Thermoforming
While thermoforming remains the standard for appliance fabrication, the inherent variability in thickness distribution is a known challenge. You might assume that these variations are designed into the treatment planning software, but most CAD algorithms still assume a uniform thickness when calculating force.
To bypass the limitations of material stretching and uneven thinning, many modern labs are transitioning toward direct 3D-printed orthodontic appliances. Direct printing allows for a truly uniform wall thickness or even variable thickness designs where the material is intentionally thicker in areas requiring high force and thinner where flexibility is needed.
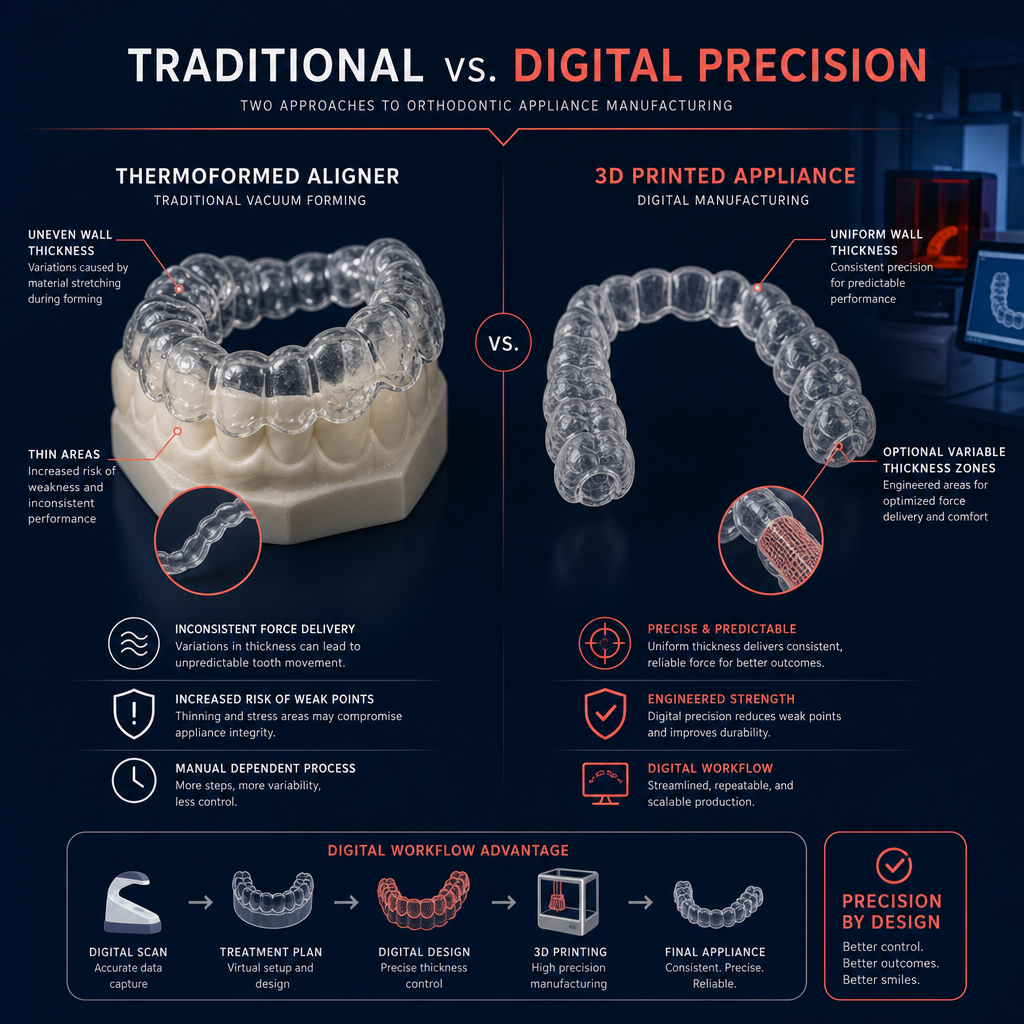
Understanding the physics of the materials you use daily ensures you can make informed decisions about material thickness and fabrication methods. If you are looking to improve the precision of your clinical outcomes, consider how the fabrication process might be altering your treatment intent.
Explore how Nordicdens leverages advanced manufacturing to ensure appliance precision – contact us today to discuss your clinic's digital production needs.
NordicDens is a modern orthodontic laboratory in Tallinn, Estonia, serving clinics across the Nordics and Europe with precision appliances and digital workflows.


